About Urology
Urology is a part of health care that deals with diseases of the male and female urinary tract (kidneys, ureters, bladder and urethra). It also deals with the male organs that are able to make babies (penis, testes, scrotum, prostate, etc.). Since health problems in these body parts can happen to everyone, urologic health is important.
Urology is known as a surgical specialty. Besides surgery, a urologist is a doctor with the wisdom of internal medicine, paediatrics, gynaecology and other parts of health care. This is because a urologist encounters a wide range of clinical problems. The scope of urology is big and the American Urological Association has named seven subspecialty parts:
- Paediatric Urology (children’s urology)
- Urologic Oncology (urologic cancers)
- Renal (kidney) Transplant
- Male Infertility
- Calculi (urinary tract stones)
- Female Urology
- Heortology (nervous system control of genitourinary organs)
Our Urological Department Offers Treatments For The Following:
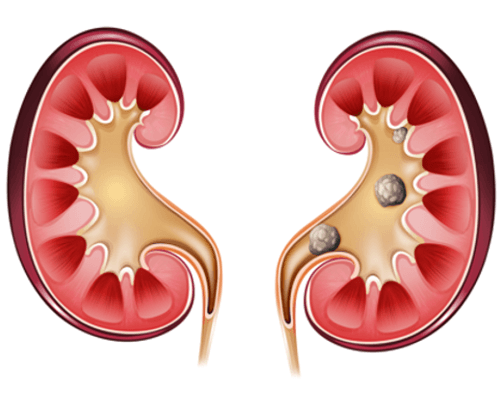
Stone Treatments
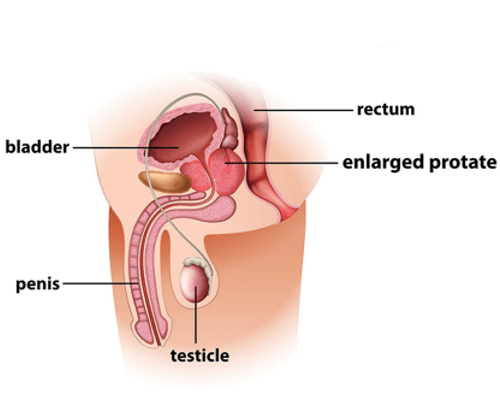
Prostate Diseases
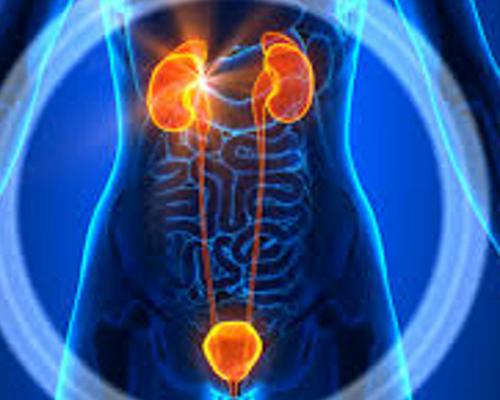
Uro-Oncology

Kidney/Ureter Stones

Bladder/ Urethral Stone

Stricture Urethra

Cancer of Bladder/ Prostate/ Penis/ Testis

Weak & Irregular Urinary System

Prostate Related Disease

Urethral Reconstructive Surgery

Cancer of Adrenal/ Kidney/ Ureter

Impotence & Sex Related Disease

Painful Micturition/ Hematuria

About Dr. Ayush Khetarpal
Dr. Ayush Khetarpal is one of the leading Urologists in Delhi. He is Certified in Urology and one of the renowned Andrologists in North India for the Past 11 Years. Dr. Ayush practices as a Consultant Urologist, Andrologist, Laparoscopic, Endoscopic and Uro-Oncosurgeon at Khetarpal Hospital, Delhi. Dr. Ayush has been involved in various publications of journals and academic chapters. His area of expertise are as follows:
– Kidney Stones
– Prostate Related Diseases
– Bladder/Urethral Stone
– Cancer of Adrenal/Kidney/Ureter
– Cancer of Bladder/Prostate/Penis/testis
– Impotence & Sex Related Diseases
– Weak & Irregular Urinary System
– Painful Micturition
Kidney Stone:
Urine contains many dissolved minerals and salts. When your urine has high levels of these minerals and salts, you can form stones. Kidney stones can start small but can grow larger in size, even filling the inner hollow structures of the kidney. Some stones stay in the kidney and do not cause any problems. Sometimes, the kidney stone can travel down the ureter, the tube between the kidney and the bladder. If the stone reaches the bladder, it can be passed out of the body in urine. If the stone becomes lodged in the ureter, it blocks the urine flow from that kidney and causes pain.
Kidneys and Urinary System
The kidneys are fist-sized organs that handle the body’s fluid and chemical levels. Most people have two kidneys, one on each side of the spine behind the liver, stomach, pancreas and intestines. Healthy kidneys clean waste from the blood and remove it in the urine. They control the levels of sodium, potassium and calcium in the blood.
The kidneys, ureters and bladder are part of your urinary tract. The urinary tract makes transports and stores urine in the body. The kidneys make urine from water and your body’s waste. The urine then travels down the ureters into the bladder, where it is stored. Urine leaves your body through the urethra.
Kidney stones form in the kidney. Some stones move from the kidney into the ureter. The ureters are tubes leading from the kidneys to the bladder. If a stone leaves the kidney and gets stuck in the ureter, it is called a ureteral stone.
Causes
– Low Urine Volume
A major risk factor for kidney stones is a constant low urine volume. Low urine volume may come from dehydration (loss of body fluids) from hard exercise, working or living in a hot place, or not drinking enough fluids. When urine volume is low, urine is concentrated and dark in color. Concentrated urine means there is less fluid to keep salts dissolved. Increasing fluid intake will dilute the salts in your urine. By doing this, you may reduce your risk of stones forming.
Adults who form stones should drink enough fluid to make at least 2.5 liters of urine every day. On average, this will take about 3 liters of fluid intake per day. While water is likely the best fluid to drink, what matters most is getting enough fluid.
– Diet
Diet can also affect the chance of forming a stone. One of the more common causes of calcium kidney stones is high levels of calcium in the urine. High urine calcium levels may be due to the way your body handles calcium. It is not always due to how much calcium you eat. Lowering the amount of calcium in your diet rarely stops stones from forming. Studies have shown that restricting dietary calcium can be bad for bone health and may increase kidney stone risk. Health care providers usually do not tell people to limit dietary calcium in order to lower urine calcium. But calcium intake should not be too high.
Instead of lowering dietary calcium intake, your health care provider may try to reduce your urine calcium level by decreasing your sodium (salt) intake. Too much salt in the diet is a risk factor for calcium stones. This is because too much salt is passing into the urine, keeping calcium from being reabsorbed from the urine and into the blood. Reducing salt in the diet lowers urine calcium, making it less likely for calcium stones to form.
A diet high in animal protein, such as beef, fish, chicken and pork, can raise the acid levels in the body and in the urine. High acid levels make it easier for calcium oxalate and uric acid stones to form. The breakdown of meat into uric acid also raises the chance that both calcium and uric acid stones will form.
– Bowel Conditions
Certain bowel conditions that cause diarrhea (such as Crohn’s Disease or ulcerative colitis) or surgeries (such as gastric bypass surgery) can raise the risk of forming calcium oxalate kidney stones. Diarrhea may result in loss of large amounts of fluid from the body, lowering urine volume. Your body may also absorb excessive oxalate from the intestine, resulting in more oxalate in your urine. Both low urine volume and high levels of urine oxalate can help to cause calcium oxalate kidney stone formation.
– Obesity
Obesity is a risk factor for stones. Obesity may change the acid levels in the urine, leading to stone formation.
– Medical conditions
Some medical conditions have an increased risk of kidney stones. Abnormal growth of one or more of the parathyroid glands, which control calcium metabolism, can cause high calcium levels in the blood and urine. This can lead to kidney stones. Another condition called distal renal tubular acidosis, in which there is acid build-up in the body, can raise the risk of calcium phosphate kidney stones.
Some rare, inherited disorders can also make certain types of stones more likely. Examples include cystinuria, which is too much of the amino acid cystine in the urine, and primary hyperoxaluria, in which the liver makes too much oxalate.
Medication
Some medications, and calcium and vitamin C supplements, may increase your risk of forming stones. Be sure to tell your health care provider all the medications and supplements you take, as these could affect your risk of stone formation. Do not stop taking any of these unless your health care provider tells you to do so.
Family History
The chance of having kidney stones is much higher if you have a family history of stones, such as a parent or sibling.
Common Symptoms Of Kidney Stones Are:
- Sharp, cramping pain in the back and side, often moving to the lower abdomen or groin. Some women say the pain is worse than childbirth labor pains. The pain often starts suddenly and comes in waves. It can come and go as the body tries to get rid of the stone.
- A feeling of intense need to urinate.
- Urinating more often or a burning feeling during urination.
- Urine that is dark or red due to blood. Sometimes urine has only small amounts of red blood cells that can’t be seen with the naked eye.
- Nausea and vomiting.
- For men, you may feel pain at the tip of the penis.
URINARY TRACT INFECTION
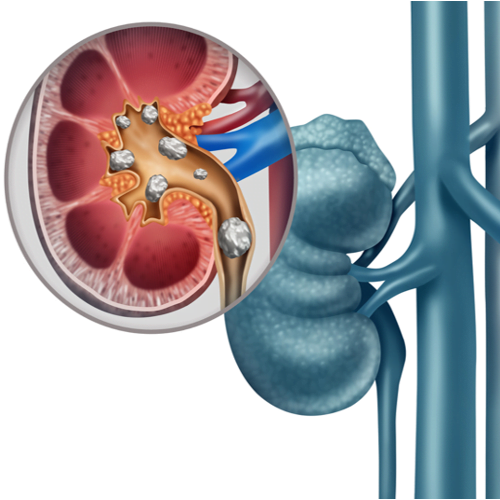
FAQs
- Why would you need to see a urologist?
You need to visit our urologist if you show signs of any infection or condition concerning your urinary tract. Some of the symptoms that suggest a problem in the urinary tract include;
- Blood in your urine
- Pain or burning sensation
- Frequent need to urinate
- Pain in your pelvis or lower back
- Men may also need to visit a urologist if you observe these symptoms
- Decreased sexual desire
- Lump in the testicle
- What are the kinds of urological problems?
Urological problems can differ mostly in men, women and children.
Men
- Cancers concerning bladder, kidneys, penis, testicles and prostate glands
- Erectile dysfunction
- Infertility
- Kidney stones
- Urinary tract infections
- Interstitial cystitis
Women
- Bladder prolapses
- Cancers concerning bladder, kidneys, and adrenal glands
- Urinary tract infections
- Urinary incontinence
- Overactive bladder
Children
- Bed-wetting
- Urinary tract structure problem
- Undescended testicles
- What diseases do urologists treat?
Urologists treat all diseases and conditions concerning the urinary tract. The diseases include;
Benign Prostatic Hyperplasia (BPH): This is a disease where the prostate gland increases in size. BPH is not directly connected to the prostate gland and is mostly observed in older men.
Urinary Incontinence: This refers to a loss of bladder control
Urinary Tract Infections (UTI’s): Pathogenic bacteria or viruses enter the urinary tract and cause infection.
Kidney Stones: Deposits are formed in the kidneys and cause mild to excruciating pain when passed through urine.
- How do you know if something is wrong with your kidneys?
Kidneys are a pair of organs that filter your blood and help remove toxins from your body. When kidneys lose the ability to filter waste from your blood a kidney failure may occur. Some of the symptoms to look out for are;
- Seizures
- Excessive fatigue
- Shortness of breath
- Nausea
- Swelling of your legs, feet and ankles
- Reduced urine flow

