About Piles
Piles or Haemorrhoids are swollen and inflamed veins in the rectum and anus which cause severe discomfort and bleeding and are usually caused by continuous straining during regular bowel movements, obesity or pregnancy. The size of piles can vary, and they are found inside or outside the anus. Piles occur due to chronic constipation, chronic diarrhea, lifting heavy weights, pregnancy, or straining when passing a stool. Discomfort is a common symptom, especially during bowel movements or when sitting. Other symptoms include itching and bleeding and a doctor can usually diagnose piles on examination.
Types Of Piles:
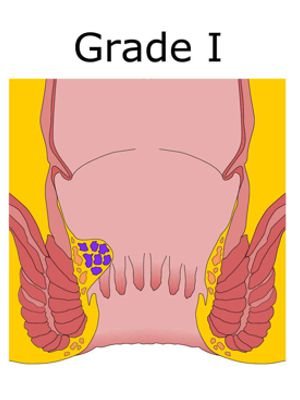
Grade -1
There are small inflammations, usually inside the lining of the anus. They are not visible.
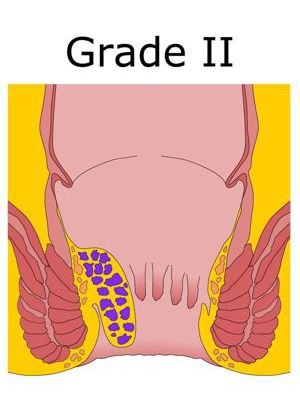
Grade - 2
Grade II piles are larger than grade I piles, but also remain inside the anus. They may get pushed out during the passing of stool, but they will return unaided.
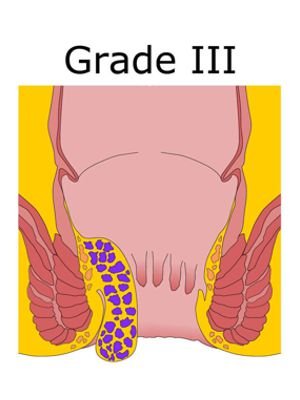
Grade - 3
These are also known as prolapsed hemorrhoids and appear outside the anus. The individual may feel them hanging from the rectum, but they can be easily re-inserted.
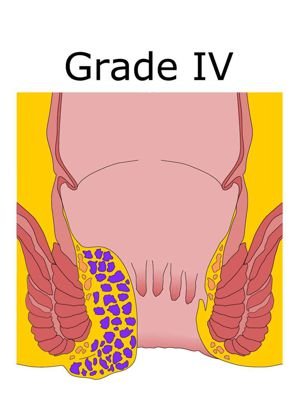
Grade - 4
These cannot be pushed back in and need treatment. They are large and remain outside of the anus.
Symptoms Of Piles:
Common piles symptoms include:
- A hard, possibly painful lump may be felt around the anus. It may contain coagulated blood. Piles that contain blood are called thrombosed external hemorrhoids.
- After passing a stool, a person with piles may experience the feeling that the bowels are still full.
- Bright red blood is visible after a bowel movement.
- The area around the anus is itchy, red, and sore.
- Pain occurs during the passing of a stool.
- excessive anal bleeding, also possibly leading to anemia or infection
- fecal incontinence, or an inability to control bowel movements
- anal fistula, in which a new channel is created between the surface of the skin near the anus and the inside of the anus
- a strangulated hemorrhoid, in which the blood supply to the hemorrhoid is cut off, causing complications including infection or a blood clot

Causes Of Piles:
- chronic constipation
- chronic diarrhea
- lifting heavy weights
- pregnancy
- straining when passing a stool
- tendency for Piles increases with age
Common Causes Include:
- Strain due to constipation while passing stool
- Physical exertion
- Strain during urination
- Chronic coughing
- Cystic fibrosis disorder
- Enlarged prostate
- Multiple pregnancies
- Being overweight Abdominal fluid
- Lifting heavy items
- Peritoneal dialysis
- Poor nutrition
- Smoking
- Undescended testicles

When To See A Doctor?
A doctor can usually diagnose piles after carrying out a physical examination. They will examine the anus of the person with suspected piles.
The doctor may ask the following questions:
- Do any close relatives have piles?
- Has there been any blood or mucus in the stools?
- Has there been any recent weight loss?
- Have bowel movements changed recently?
- What color are the stools?
For internal piles, the doctor may perform a digital rectal examination (DRE) or use a proctoscope. A proctoscope is a hollow tube fitted with a light. It allows the doctor to see the anal canal up close. They can take a small tissue sample from inside the rectum. This can then be sent to the lab for analysis.
The physician may recommend a colonoscopy if the person with piles presents signs and symptoms that suggest another digestive system diseases, or they are demonstrating any risk factors for colorectal cancer.
Treatment Options For Piles:
Banding: The doctor places an elastic band around the base of the pile, cutting off its blood supply. After a few days, the hemorrhoid falls off. This is effective for treating all hemorrhoids of less than grade IV status.
Sclerotherapy: Medicine is injected to make the hemorrhoid shrink. The hemorrhoid eventually shrivels up. This is effective for grade II and III hemorrhoids and is an alternative to banding.
Infrared coagulation: Also referred to as infrared light coagulation, a device is used to burn the hemorrhoid tissue. This technique is used to treat grade I and II hemorrhoids.
Hemorrhoidectomy: The excess tissue that is causing the bleeding is surgically removed. This can be done in various ways and may involve a combination of a local anesthetic and sedation, a spinal anesthetic, or a general anesthetic. This type of surgery is the most effective for completely removing piles, but there is a risk of complications, including difficulties with passing stools, as well as urinary tract infections.
Hemorrhoid stapling: Blood flow is blocked to the hemorrhoid tissue. This procedure is usually less painful than hemorrhoidectomy. However, this procedure can lead to an increased risk of hemorrhoid recurrence and rectal prolapse, in which part of the rectum pushes out of the anus.
FAQs
- Can blood in my stool area be harmless?
Blood in your stool can indicate different kinds of problems. We advise a consultation with our expert hernia doctors to diagnose the problem. It could be Piles/Hemorrhoids.
- Can Piles be naturally treated?
Piles/Hemorrhoids detected at a very early stage can be naturally treated. However, in cases where there is pain and bleeding, surgery will be required. Maintain a high-fibre diet to get relief.
- Should I go for Piles surgery?
Surgery is a must in aggravated cases where there is a lump felt in the anus, sore or painful anus, bleeding, or severe pain.
- How much time will the surgery take?
The recovery from a hemorrhoid treatment or surgery typically lasts one to six weeks, depending upon the type of treatment, the severity of the hemorrhoids, and the number removed.
- Is it possible for the Piles to reappear?
Hemorrhoids can reoccur on and off for various reasons—sometimes related to lifestyle habits, and sometimes due to a medical condition.
- When can I resume daily activities after the surgery?
Most patients begin to feel better at the end of the first week, especially if the patient is able to keep their bowel movements soft or slightly loose and can resume daily activities.

